A muscle-sparing approach to hip replacement designed to restore mobility, relieve pain, and support a structured recovery.
Most patients seek hip replacement after months or years of progressive pain that limits mobility and quality of life. Total hip replacement addresses advanced arthritis and joint degeneration when conservative treatment is no longer effective.
As part of Watauga Orthopaedics, joint replacement care is delivered in coordination with our regional orthopedic team.
Anterior Hip Replacement
What Is Anterior Total Hip Replacement?
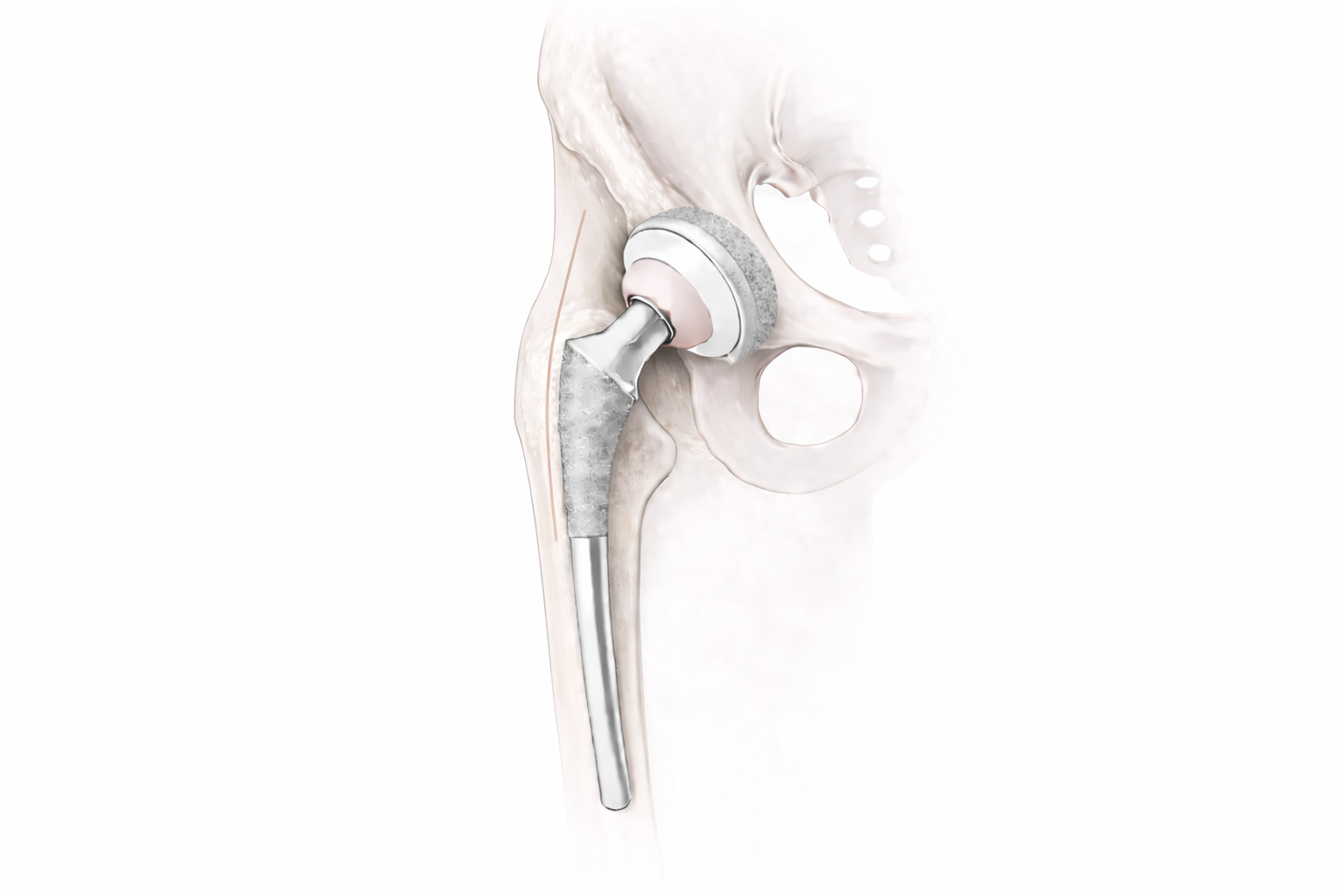
Total hip replacement removes damaged cartilage and bone from the hip joint and replaces them with precision-engineered components designed to restore smooth, stable motion.
In appropriate patients, the procedure is performed between muscles rather than splitting or detaching them. Preserving surrounding soft tissue may support early mobility and stability within a structured recovery plan.
The goal is not simply surgery — it is durable pain relief, restored function, and a safe return to daily activity.
Anterior Hip Replacement:
Key Points
Who is a candidate?
Patients with hip arthritis who have persistent pain, stiffness, or functional limitation despite non-operative treatment.
Is this an outpatient procedure?
Most anterior hip replacements are performed in an outpatient setting, allowing patients to return home the same day.
What are the benefits of the anterior approach?
A muscle-sparing technique that may allow for faster early recovery, improved stability, and a more natural return to activity.
How long is recovery?
Patients typically walk the same day, with meaningful improvement over the first few weeks and continued progress over several months.
What are the risks?
Infection, blood clots, implant wear, and other rare complications related to surgery.
Hip Replacement on X-Ray
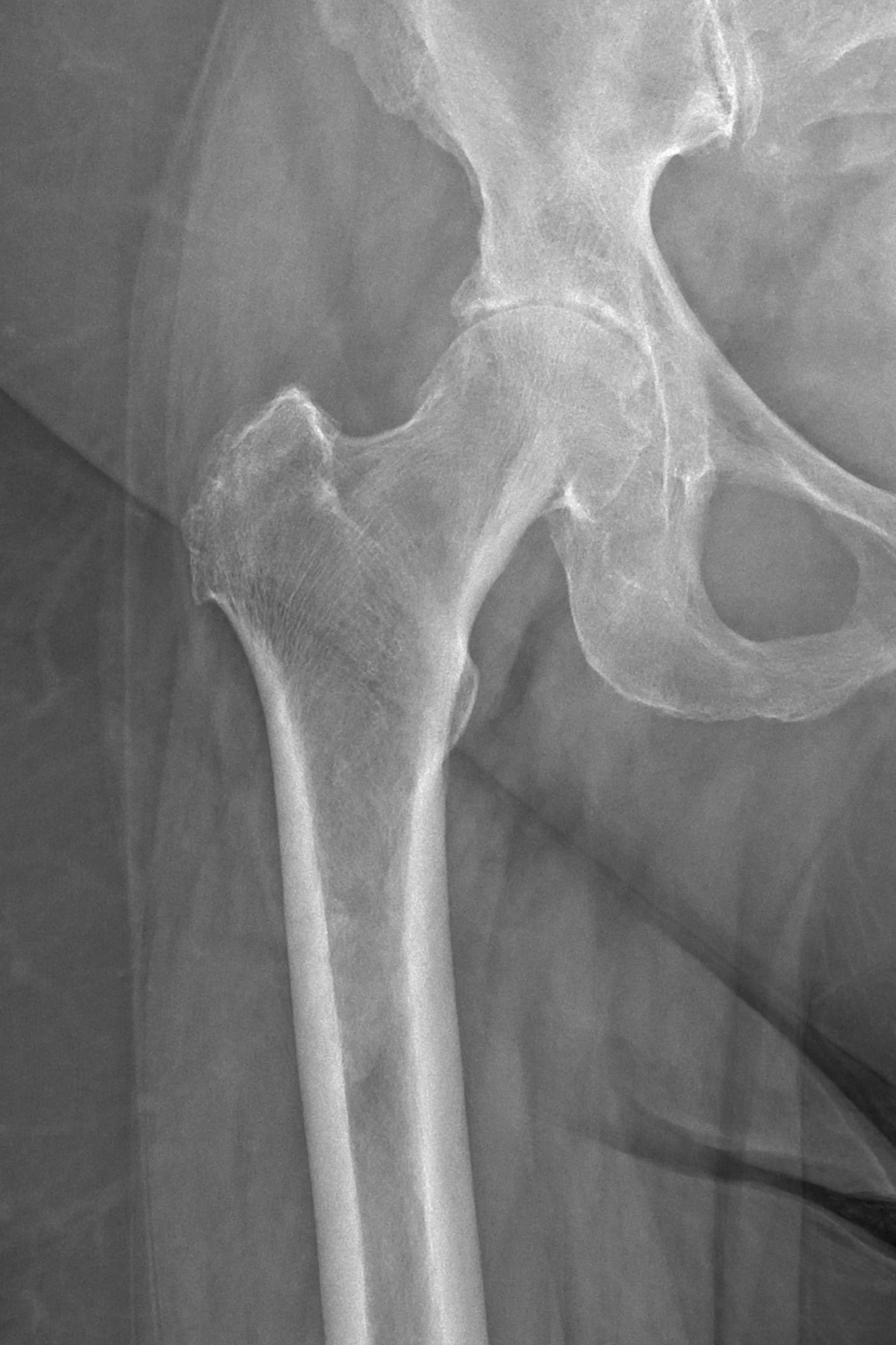
Before Surgery
Advanced degenerative arthritis
Preoperative X-rays often demonstrate joint space narrowing, bone-on-bone contact, osteophyte formation, and deformity related to advanced arthritis.
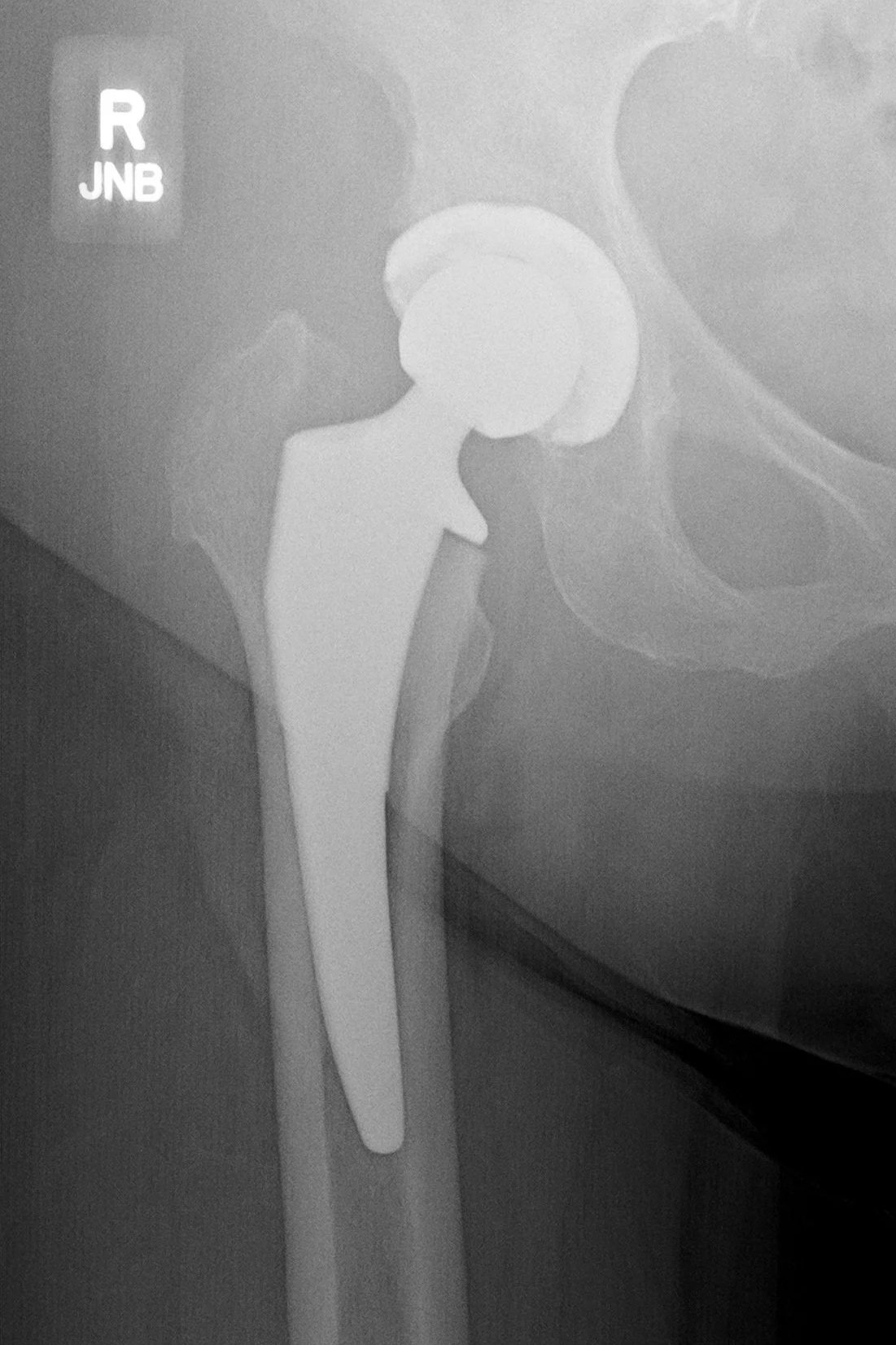
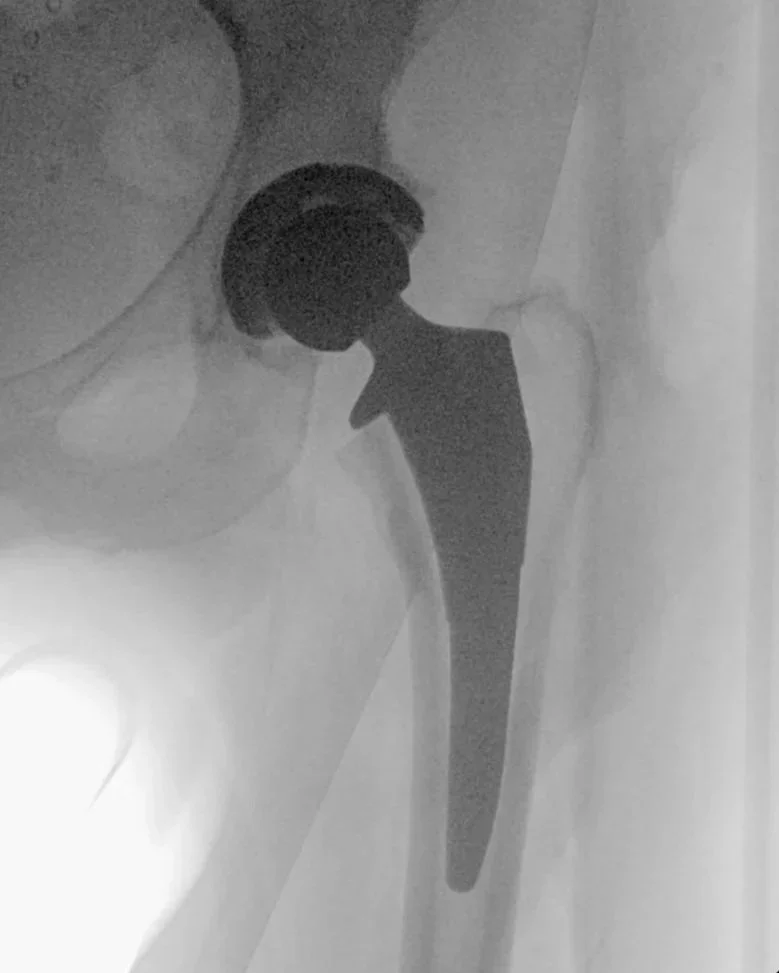
After Surgery
Total hip replacement
After total hip replacement, the damaged joint surfaces are replaced with precision-positioned components. The acetabular cup and femoral stem restore alignment, stability, and joint mechanics.
Who Is a Candidate?
Anterior total hip replacement may be appropriate for patients with advanced degenerative conditions of the hip, including:
Osteoarthritis
Avascular necrosis
Inflammatory arthritis
Post-traumatic arthritis
Not every patient is best served by the same surgical approach. A comprehensive evaluation — including imaging review and discussion of recovery expectations — helps determine the safest and most reliable surgical plan.
Surgical Team & Joint Replacement Center

Dedicated Joint Replacement Team
Board-certified orthopedic surgeon
Experienced operating room personnel
Anesthesia team experienced in regional and multimodal techniques
Coordinated perioperative nursing care
Outpatient Joint Replacement at an Accredited Center of Excellence
Watauga Orthopaedics Center for Advanced Bone and Joint Surgery
AAAHC-accredited Center of Excellence for Joint Replacement
Structured same-day discharge protocols
Coordinated Recovery Pathway
Structured postoperative follow-up
Physical therapy coordination
Direct access for clinical concerns
Individualized recovery oversight
Personalized Evaluation. Structured Plan.
Many patients seek consultation after months of progressive hip pain that limits daily activity. Every patient’s anatomy, activity level, and goals are different.
A consultation allows us to review imaging, discuss non-surgical options, and outline a plan tailored to you.
Evaluation
A comprehensive history, examination, and imaging review guide treatment. When surgery is appropriate, planning is individualized based on anatomy, health status, and functional goals.
What to Expect
Preparation
Medical optimization, patient education, and a defined recovery plan help ensure readiness and support a smooth perioperative course.
Surgery
Anterior total hip replacement is performed using modern planning and evidence-based protocols. Precise component positioning and soft-tissue preservation are priorities. Many patients undergo surgery in an outpatient setting with same-day discharge when appropriate.
Recovery
Mobilization begins the day of surgery. Structured rehabilitation and scheduled follow-up visits support steady improvement in pain, mobility, and function over the first several weeks.
Results
Significant pain reduction
Improved mobility and daily function
High long-term patient satisfaction in contemporary studies
Durable performance over time
Smooth recovery for most patients with steady improvement during the first several weeks
Clinical Outcomes
Risks
Infection
Blood clots
Fracture
Instability
Leg length difference
Nerve injury
Implant wear or loosening
Surgical planning is individualized to anatomy, bone quality, overall conditioning, and functional demands.
Recovery Timeline

Day of Surgery
Walking begins within hours after hip replacement.
Weeks 1–2
Focus on mobility, wound care, and safe movement at home.
Weeks 2–6
Return to driving and activity as gait and confidence improve.
Weeks 6–12
Progression of strength and endurance. Return to work.
3+ Months
Return to higher-level activity as recovery matures.
1 Year
Strength, balance, and function fully established.
Frequently Asked Questions
-
Modern pain control strategies, including regional anesthesia and multimodal medications, significantly reduce postoperative discomfort. Most patients report rapid improvement in arthritic pain and manageable surgical soreness during the first few weeks.
-
Most patients resume basic daily activities within a few weeks. Strength, endurance, and function continue improving over several months, with full recovery progressing over the first year.
-
Walking typically begins within hours of surgery. Early mobilization supports circulation, strength, and overall recovery.
-
Driving depends on the side of surgery, medication use, and confidence with mobility. Many patients return to driving within 2–6 weeks once they are off narcotic medication and able to react safely.
-
Restrictions are individualized. With modern anterior approaches, formal hip precautions are often minimized. Safe movement techniques are reviewed before discharge.
-
Yes. Many patients undergo hip replacement in an accredited ambulatory surgery center and return home the same day when medically appropriate.
-
The difference lies in how the hip joint is accessed. The anterior approach uses a muscle-sparing interval in the front of the hip, which may reduce early muscle disruption and facilitate recovery. Implant durability and long-term outcomes are comparable when performed properly.
-
Modern implants demonstrate over 90% survivorship at 20 years in large studies. Longevity depends on activity level, bone quality, and overall health.
-
Risks include infection, blood clots, fracture, instability, leg length discrepancy, nerve injury, and implant wear over time. Careful surgical planning and structured recovery protocols are designed to minimize these risks.
-
Most patients benefit from guided physical therapy to restore strength and mobility. The specific program is individualized based on progress and goals.
-
Many patients living alone successfully undergo hip replacement. Planning ahead for short-term assistance during the first several days is important and discussed before surgery.
Ready to Discuss Your Options?
A structured evaluation helps determine whether surgery is appropriate and how to approach it safely.
If hip pain is limiting your mobility, we will review imaging, discuss non-surgical options when appropriate, and outline a plan aligned with your goals.